Hundreds of thousands of people are hospitalized for a traumatic brain injury (TBI) in the United States each year, with millions more impacted worldwide. There is still so much to learn about TBI and the way it can change somebody’s life. What research is indicating now is that people who have a TBI are at risk for struggling with chronic pain.
Today, we’ll be able to look deeper into the connection between TBI and chronic pain. We’ll have the answers to your questions about this condition, giving you more insight into all the ways a traumatic brain injury can leave you with chronic concerns.
What Is a Traumatic Brain Injury?

A traumatic brain injury (TBI) is much more than a bump to the head; it happens when the brain is jostled in the skull. Even just a minor head injury can burst blood vessels and damage brain tissue, which can lead to brain bleeding.
This shows that a TBI can very easily result in permanent damage to the brain. There are many different ways that a TBI can occur, such as:
- A blow to the head
- A motor vehicle accident
- A fall
- Self-inflicted gunshot wound
- Being tackled in sports
- And more
Though anybody can get a TBI, certain risk factors increase the chances of this occurring. For example, people who play high-contact sports (such as football) are at a much greater risk of receiving a TBI. Additionally, older adults make up a large percentage of those who require hospitalization because of a TBI. The same goes for children who receive a head injury because of how greatly it can impact their development.
Upon receiving a TBI, people can experience loss of consciousness, vomiting, blurred vision, and more. After the initial trauma, symptoms of a TBI can range widely, including concerns such as:
- Headaches
- Memory loss
- Difficulty concentrating
- Cognitive impairments
- Insomnia
- Speech challenges
- Fine- and gross-motor skill deficits
- Nerve damage
- Chronic pain
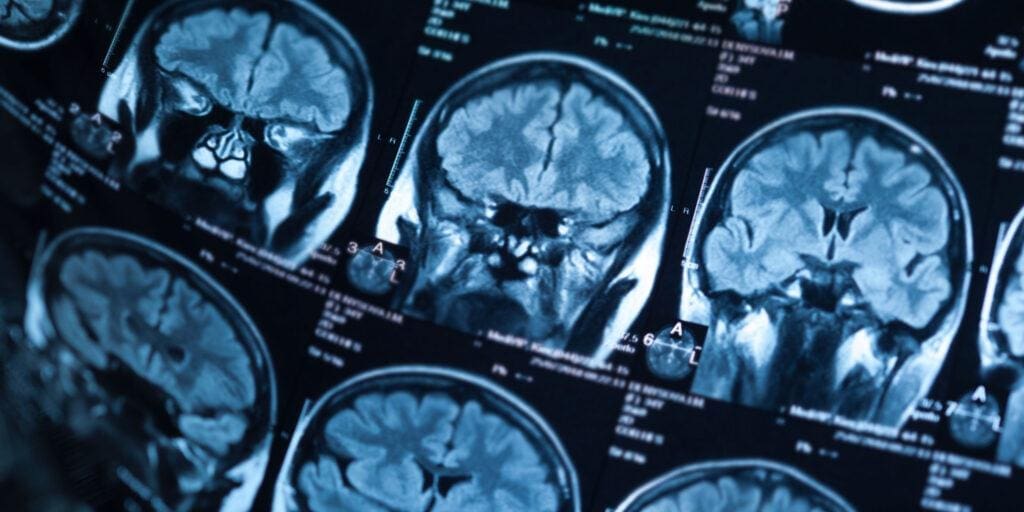
A TBI is diagnosed through a neurological evaluation of the patient’s symptoms combined with imaging. A computed tomography (CT) scan or a magnetic resonance imaging (MRI) scan can sometimes be effective in determining the severity of the TBI. This is usually done in conjunction with something called the Glasgow Coma Scale (GCS). The GCS goes through how a patient responds physically, verbally, and cognitively to certain stimuli.
According to the Centers for Disease Control and Prevention (CDC), TBIs are typically classified as mild (also known as a concussion), moderate, or severe based on the GCS score. These classifications dictate how impactful the TBI is on the person’s ability to function. But even a mild traumatic brain injury can negatively impact somebody’s quality of life. This is especially true in cases where a TBI leads to long-lasting chronic pain.
Can a Traumatic Brain Injury Cause Chronic Pain?
Studies show that more than half of patients who are diagnosed with a mild TBI report having chronic pain after the incident. But why is this the case? And how do you know if your TBI is what’s causing your chronic pain?
It’s important to note that, not only can a head injury result in pain at the site, but brain damage can also disrupt the pain receptors in the brain. Usually, the nerves throughout the body send signals to the brain when there’s distress, an injury, an illness, etc. But sometimes, these pain receptors can overreact, causing the brain to perceive more pain than usual. This means that if you already had chronic pain or a condition that causes discomfort before the TBI, you might be more sensitive to the side effects of that condition now.
Furthermore, any damage to the brain can cause a domino effect throughout the body. When the systems of the body are not able to work at full capacity as a result of a TBI, there can be serious side effects. These side effects might look like:
- Muscle spasms
- Stomach pain
- Migraines
- Nerve pain
- Numbness and tingling
- Depression or other mental health concerns
These are just some examples of how a TBI can change the way that the body works. Very frequently, people who have been diagnosed with a TBI are documented as also experiencing head, neck, and back pain. This pain often lingers long after the initial injury.
Having a TBI can also change one’s ability to move or exercise as they would before. It’s essential to always follow the recommendations of your doctor before beginning to exercise again after a TBI. You might need to change up your exercise routine to match your body and brain’s abilities. Some people even need accommodations at work after receiving a TBI because of the pain and discomfort it brings to them.
The way that you respond to a TBI will depend on the level of severity of the injury. Moreover, how you feel doing certain activities that may strain the brain (reading, working, exercising, and so forth) can influence what you do to address the symptoms.
Can Chronic Pain from a TBI Be Treated?

In truth, there are not many cutting-edge treatments for a TBI and its side effects, especially when the case is mild. Often, getting plenty of rest is the biggest way to see improvement for a TBI. This might mean taking it easy, catching up on sleep, and possibly taking a break from electronic devices so as not to strain the eyes and brain. Also, research indicates that abstaining from using drugs or drinking alcohol can help to keep you on track toward recovery.
Other ways to help with the pain that comes from a traumatic brain injury would be to:
- Take over-the-counter or prescribed pain medication
- Try natural remedies for pain
- Do cognitive behavioral therapy (CBT)
- Do physical therapy
Most importantly, one of the most helpful things you can do with a traumatic brain injury is connect with others who understand the frustrations, pain, and long-lasting side effects. See what others are sharing about their own experiences with chronic pain through the Pain Resource Community online.
What Are Your Thoughts on TBI?
Let us know in the comments below!
What Chronic Pain Topics Should We Cover Next?
Email us your ideas at info@painresource.com
Join the Pain Resource Community
Did you know the Pain Resource Community has different groups for different conditions? Connect with others who share the same condition as you here.




