Chronic foot pain can be extremely aggravating to live with. Think of how often you’re on your feet throughout the day. Now, add in a burning, stinging sensation that’s accompanied by cracked or flaking skin, and just like that your seemingly innocuous morning stroll is out of the question. One of the most common causes of foot pain is a fungal infection known as athlete’s foot. Given the name, if you’re not an athlete, or if you live a more sedentary lifestyle, you may not think you’re at risk. This is simply not the case. Athlete’s foot can occur to anyone at any time, which is why it’s important to understand this common skin condition. Below, we’ll cover everything you need to know about athlete’s foot, and what you can do to reduce your risk.
What Is Athlete’s Foot?
Athlete’s foot, known scientifically as tinea pedis, is a contagious fungal infection that usually occurs between the toes. The fungus that causes athlete’s foot is called Trichophyton and is commonly found on floors and in clothing. The condition typically occurs in people whose feet have become very sweaty while confined within tight-fitting shoes. In some cases, the condition can spread to the tonsils, feet, and hands, although this is not as common.
Athlete’s foot is one of the most common types of fungal skin infections. It’s estimated that around 15 to 25 percent of the population. Athletes, males, and older individuals are more likely to develop the condition.
Athlete’s foot is closely related to other fungal infections like ringworm and jock itch. For most people, athlete’s foot isn’t serious, but oftentimes it can be hard to cure. It can be treated with antifungal medications, but the infection often comes back soon after a regimen has been completed. Individuals with a weakened immune system or diabetes should see a doctor as soon as athlete’s foot develops, as the condition can become serious.
What Causes Athlete’s Foot?

As previously mentioned, athlete’s foot is caused by the same type of fungi (dermatophytes) that cause ringworm and jock itch. You can catch this fungus through direct contact with an infected person, or by touching surfaces contaminated with it. The fungus thrives in warm, moist environments, which is why it develops mainly between the toes, and in people who wear more tight-fitting shoes. It’s commonly found in showers, on locker room floors, and around swimming pools. Rarely, athlete’s foot can be caused by non-dermatophytes, like yeast (candida).
Athlete’s foot is mildly contagious. Walking barefoot may increase your chances of contracting the fungus. Your risk of developing athlete’s foot may also depend on your susceptibility. For example, people who have an impaired immune system or diabetes are at greater risk of infection if they have an open cut or sore on their feet.
Immunocompromised individuals and those with diabetes aren’t the only ones who are at greater risk of developing athlete’s foot. Next, we’ll cover the most common risk factors for athlete’s foot, and explain how you can minimize your risk.
Who’s At Risk?
Contrary to the name, anyone can get athlete’s foot, not just athletes. However, certain behaviors, lifestyles, and professions can increase your risk. Common risk factors include:
- Wearing tight, closed-toe shoes
- Having sweaty feet
- Keeping your feet wet for long periods
- Visiting public places barefoot, especially locker rooms, swimming pools, or showers
- Sharing socks, shoes, or towels with an infected person
- Having a minor skin or nail injury on your foot
- Playing sports frequently
It’s important to understand what can cause athlete’s foot, as it can help you avoid situations that may put you at risk. For people who play sports, wear tight-fitting shoes frequently, or have sweaty feet, taking frequent breaks and airing out your feet can be a great way to reduce your risk. Other ways you can reduce your risk include:
- Wash your feet with soap and water every day
- Wear socks made of breathable fabrics
- Avoid being barefoot in public spaces
- Use antifungal powder on your feet
- Wear breathable shoes
Reducing your risk is important, but it’s also important to understand the signs and symptoms of athlete’s foot. Spotting the signs early can help you prevent spreading the fungus to other people, and get you on a treatment regimen before it becomes severe.
Athlete’s Foot Symptoms
Athlete’s foot can affect one or both feet. Typically, the condition affects the skin between the toes, although it can spread to other parts of the body, mainly the feet and hands. Other common bacterial infections can sometimes occur alongside the condition. This usually happens when athlete’s foot becomes severe and causes open sores in the skin, making it more vulnerable to bacteria.
Some of the common symptoms of athlete’s foot include:
- Itchy, scaly red rash between your toes
- Small, red blisters (usually on your soles or between your toes)
- Ongoing dryness and scaling on the soles and up the sides of your feet
- Ulcers or sores that leak fluid, smell bad, and look red
- Discolored, thick, and fragile toenails
- Toenails that pull away from your nail bed
- Raw skin on your feet
If you notice any of the above-mentioned signs, or if you believe you may be at risk for athlete’s foot, talk with your doctor about what your next steps should be. Your doctor may be able to diagnose you simply based on your symptoms, or they may order a skin test if they aren’t sure of the cause. Once you have a diagnosis, your doctor will likely start you on a treatment regimen.
Treatment for Athlete’s Foot
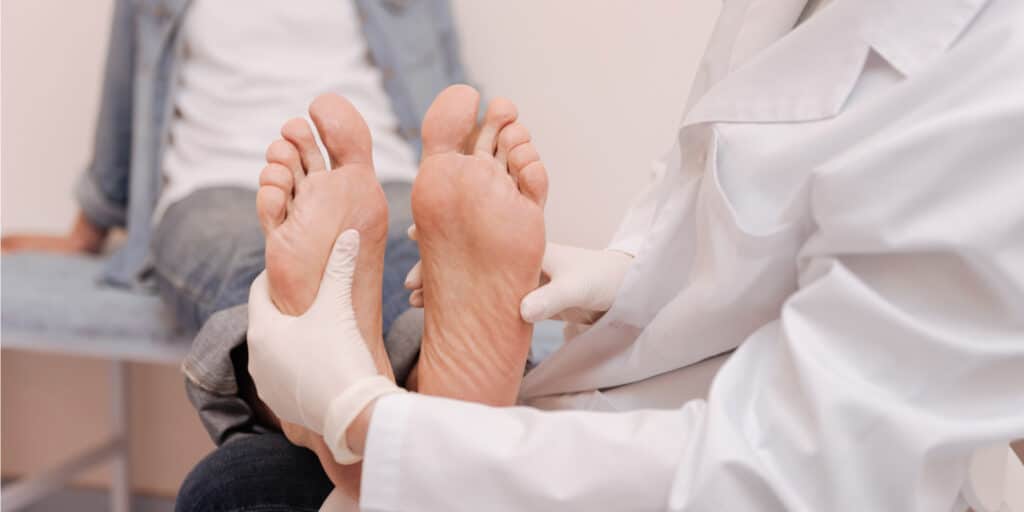

In the majority of cases, athlete’s foot symptoms are mild, and you may not require seeing a doctor. Due to this, athlete’s foot can often be treated with over-the-counter (OTC) topical antifungal medications. These can include lotions, creams, or sprays and can be found at most pharmacies or drug stores. Common OTC antifungals include:
- Miconazole (Desenex)
- Terbinafine (Lamisil AT)
- Clotrimazole (Lotrimin AF)
- Butenafine (Lotrimin Ultra)
- Tolnaftate (Tinactin)
Should OTC medications not be successful, your doctor may prescribe topical or oral prescription-strength antifungal medications. They may also recommend at-home treatments and prevention methods to help mitigate your risk for reinfection. Some of the prescription medications your doctor may prescribe include:
- Topical, prescription-strength clotrimazole or miconazole
- Topical steroids to reduce inflammation
- Oral antifungals such as itraconazole (Sporanox), fluconazole (Diflucan), or prescription-strength terbinafine (Lamisil)
- Oral antibiotics should other bacterial infections occur
Home care for athlete’s foot can include things like soaking your feet in salt water or diluted vinegar to help with blisters. Other alternatives include using tea tree oil, or other similar products to help with infections.
Do You Struggle with Athlete’s Foot?
Tell us your experiences in the comments section below!
What topics related to chronic foot pain should we cover next?
Email us your ideas at info@painresource.com, we may just feature your idea in a future article!
Living with athlete’s foot? Looking for a support group?
Join the Pain Resource Community today to start connecting with other people just like you!




