If you suffer from chronic pain, you’re no stranger to the question, “where does it hurt?” While this question is a natural starting point for diagnosis, not everyone’s experience with chronic pain is the same. Pain is complicated, and it can vary significantly between individuals. This can make it difficult to explain and quantify your pain when talking with your doctor. Thankfully, a recent study has found that there are nine types of chronic pain, each with its unique symptoms and areas on the body. Not only can this help you better understand your pain, but it can also help you articulate your pain to your doctor.
So, what are the nine types of chronic pain, and where are they located on the body? Here’s what you need to know.
What are The Nine Types of Chronic Pain?
 A recent study, published in the journal PLOS ONE, found that the body has nine distinct types of chronic pain. According to the study, the pain distribution reported by a patient is enough on its own to predict a host of other information. This includes pain intensity, impact, and even how well you’ll be faring three months after treatment. Put simply, if a patient can accurately describe and pinpoint their pain to a doctor or specialist, their chances for a successful recovery are significantly higher.
A recent study, published in the journal PLOS ONE, found that the body has nine distinct types of chronic pain. According to the study, the pain distribution reported by a patient is enough on its own to predict a host of other information. This includes pain intensity, impact, and even how well you’ll be faring three months after treatment. Put simply, if a patient can accurately describe and pinpoint their pain to a doctor or specialist, their chances for a successful recovery are significantly higher.
During their study, scientists at the University of Pittsburgh examined data from over 21,500 people who had visited the university’s severe pain management clinic. Using a specialized computer that can map patients’ pain on the body, the team found that all of the patients fit into nine distinct groups of chronic pain.
“We found that how a patient reports the bodily distribution of their chronic pain affects nearly all aspects of the pain experience, including what happens three months later,” said Dr. Benedict Alter, Assistant Professor and Director of Translational Pain Research at the University of Pittsburgh and the study’s lead author.
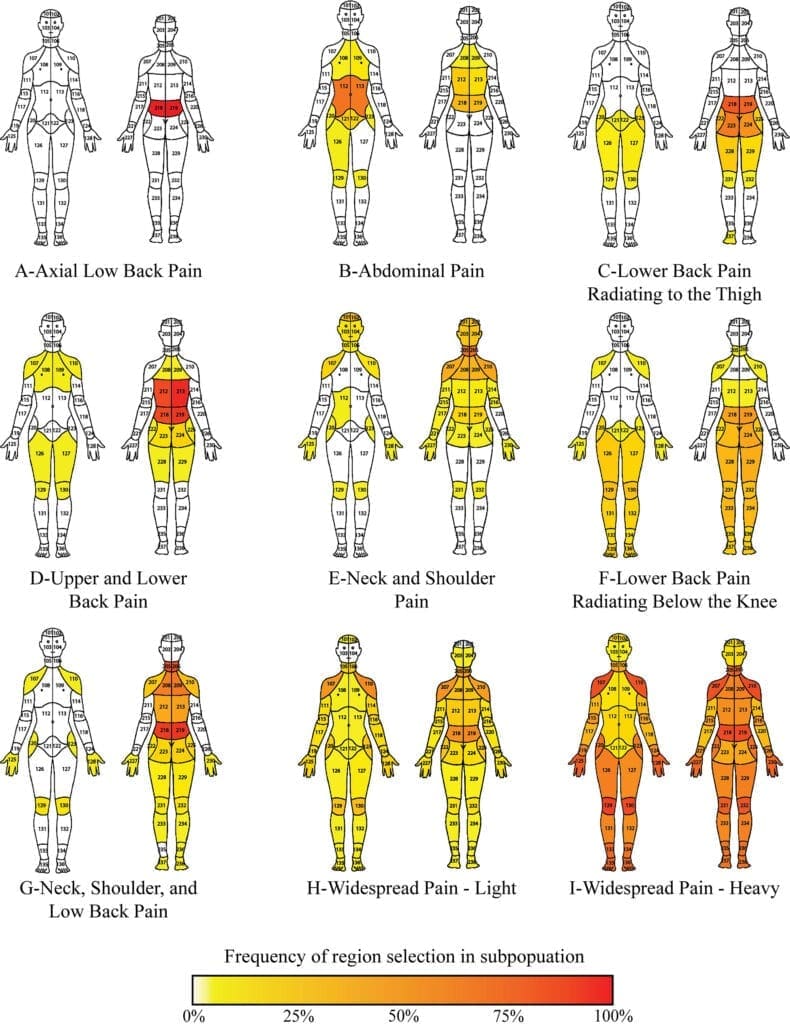
The study also noted that these patterns of pain distribution could also predict pain intensity, pain quality, pain impact, physical function, mood, sleep and indicate likely patient outcomes. Below are the nine types of chronic pain found in the study, along with their symptoms and locations.
Axial Low Back Pain (Group A)
Axial low back pain was the least commonly reported of the nine types of chronic pain, with only 677 patients reporting pain in this area. This type of pain is located in the lower back, right above the glutes. While axial low back pain was the least common of the nine types of chronic pain, patients who reported pain in this area did so at a near 100 percent rate. As noted in the diagram, patients who reported axial low back pain also reported no other pain in the body, making it the most localized of the nine.
Abdominal Pain (Group B)
Abdominal pain is pain that originates in the abdomen area. Patients who reported suffering from abdominal pain showed the highest likelihood of recovery, with nearly 49 percent reporting improvement in their symptoms three months after the study. Individuals who reported pain in their abdomen also reported pain in areas such as the lower back, upper chest, and right leg, at a rate of about 25 percent.
Lower Back Pain Radiating to the Thigh (Group C)
Of the nine types of chronic pain, only two involved pain that “radiated.” The term radiate refers to pain that originates from one part of the body and travels to another. In the case of group C, lower back pain radiating to the thigh is just as it sounds. This group of patients reported pain starting in the lower back, which then traveled down either one or both of their thighs. Important, this type of pain stopped at the knee for nearly all patients.
Upper and Lower Back Pain (Group D)
Patients in group D reported pain in both their upper and lower back, with some reporting pain in their shoulders and thighs. This group had the second-highest average pain intensity score of about six and a half out of ten.
Neck and Shoulder Pain (Group E)
Neck and shoulder pain, as the name suggests, is pain located in the neck, shoulders, and upper back area. Patients who reported suffering from neck and shoulder pain, as shown in group E, had the highest levels of physical function. This means that individuals in this group suffered the least amount of physical limitations when compared to the other eight groups. Interestingly, a small number of patients, around 25 percent, who reported neck and shoulder pain also reported pain in their knees.
Lower Back Pain Radiating Below the Knee (Group F)
This type of chronic pain was the most common of the nine, with 6709 individuals reporting symptoms in this area. This type of pain, given the name, is pain that originates in the lower back, that then travels down the legs, however, unlike group C, this pain travels below the knee. Aside from group I, group F scored the highest in several different categories. These include level of reduced physical function, sleep disturbance, and pain interference.
Neck, Shoulder, and Low Back Pain (Group G)
Those who fell in the neck, shoulder, and low back pain category were patients who reported pain in all three areas simultaneously. Patients in this group were the least likely to see improvements in their symptoms, with only 37 percent reporting an improvement at the three-month mark.
Widespread Pain Light (Group H)
Light widespread pain is pain that is reported across the body, rather than one or two specific regions. During the study, patients who were classified as having light widespread pain reported pain in an average of about 15 different body regions. The most common areas where their pain was reported were the shoulders, knees, and lower back.
Widespread Pain Heavy (Group I)
Widespread pain classified as heavy is a type of pain that affects the entire body, with a much higher intensity than that of light widespread pain. During the study, widespread pain that was determined to be “heavy” affected an average of about 30-35 different body regions. These regions could be anywhere from head to toe but were most common in the shoulders, lower back, knees, legs, feet, and hands. Patients in this group also reported the highest pain intensity, sleep disturbance, and rate of depression.
Utilizing the Nine Types of Chronic Pain


For example, while the group of patients experiencing lower back pain radiating below the knee (group F) had worse physical function difficulties than those experiencing neck and shoulder pain (E) or neck, shoulder, and lower back pain (G), these patients reported less anxiety, depression, and sleep disturbance than the other two groups. Understanding the symptoms that can accompany certain types of pain can help doctors find treatments that work more effectively for different people.
Following the study, 7,000 patients completed a follow-up questionnaire three months after the initial study. Patients experiencing abdominal pain (group B) showed the most progress, with almost half reporting significant improvement. Those with neck, shoulder, and lower back pain (group G), however, demonstrated the worst outcomes on follow-up, with only 37 percent reporting improvements.
While these results are promising, Alter and his colleagues urge caution, stating, “The definitive relationship of body map cluster assignment and pain pathophysiology remains to be seen, and even within accepted diagnoses lies significant differences in patient characteristics.”
However, they say, “given its speed and ease of use for patients, we predict that body map cluster assignment will be a useful component of chronic pain biosignature development.”
With up to 40 percent of adults in the US currently experiencing chronic pain – which is likely to increase with the potential impacts of long-term COVID-19 – diagnostic tools such as the nine types of chronic pain could make a massive difference in many people’s lives.
What are the Methods You Use for Dealing With Chronic Pain?
Let us know in the comments section!
Have a topic related to chronic pain you’d like to see us research and discuss?
Let us know by emailing us at info@painresource.com.
Are you a member of our Chronic Pain Community?





I fall into the I, C, E category plus others not listed here. But nerve pain, joint and muscle are different. This is interesting to me, if this is the locations guide that most M.D.s use, and not thinking outside of the box, this may explain many dangerous misdiagnoses. My medical mystery is mostly solved, yet still ongoing, 13 years in, and I have indeed been medicated and diagnosed incorrectly repeatedly, simply because I don’t fit into their boxed ideas. Personal research is the only reason I have a portion of my medical mystery solved and I am a big fan of researching. If a doctor tells you to not look up your symptoms, run!
Very interesting and informative article. Thank you for sharing.
I’m definitely an I. I was diagnosed with fibromyalgia this year. I do mostly have pain in my hands, feet, lower back, legs, ribs and also the hip region. When I get bad flare ups the fatigue is awful because pain is widespread.
I did find that certain foods high in histamine effect me more.
I’ve given up so many foods to calm my body. I am down to fish and chicken, fresh fruits and veggies, nothing canned. It seems that foods that are canned produce more histamine in my body. That is when I usually have a major flare. Veggies in the nightshade group also will trigger a flare.
Foods with Gluten are also a big trigger. What makes it difficult is with the cost of food going up, it’s getting harder to afford the healthier foods. So it becomes hit and miss and flares can be debilitating at those times. I’ve also suffered with pain a fatigue since I was young. Now in my 50’s after my battle with Covid Jan 2020, that was when my body pain and fatigue reached a new horrible level. Since then I’ve had the vaccines and diagnosed with fibromyalgia. It’s been a tough journey but I’m learning more about managing pain with food, filtered water intake and moderate exercise.
Lymphatic system plays a major role in keeping a healthy balance towards inflammation in the body. I’ve learned so much in 2 years and I have much more to learn.