The number of invisible illnesses that millions fight around the world is staggering. The suicide disease, as trigeminal neuralgia is commonly known, is one of those illnesses. I’m one of the approximately 12 per 100,000 per year who have been diagnosed with it.
“that affects the trigeminal or 5th cranial nerve, one of the most widely distributed nerves in the head.”
To describe the extent of the pain and debilitation trigeminal neuralgia causes seems impossible. It’s a form of chronic pain “that affects the trigeminal or 5th cranial nerve, one of the most widely distributed nerves in the head.” It’s a type of neuropathic pain “that causes extreme, sporadic, sudden burning or shock-like facial pain that lasts anywhere from a few seconds to as long as two minutes per episode.” Beyond the intense physical pain, these attacks drain those of us who suffer both mentally and emotionally. They can render us helpless as we try to manage our day-to-day lives.
My Trigeminal Neuralgia Pain Experience
When pain attacks me, I first feel it just under my right cheekbone. Then it moves into the right eye socket and into my right sinus cavity. I’ve lived with trigeminal neuralgia flare-ups for almost 14 years now, but they were once so few and far between that I didn’t know of a name to put with them.
They were easy to brush them off: maybe a sinus thing or maybe even a dental thing, I rationalized. They were sporadic and would leave quickly, so I focused on my other chronic health conditions. But when I began to have more frequent and intense flare-ups this year, I was forced to confront the issue.
My Trigeminal Neuralgia Treatment Journey

I began my prescription journey with carbamazepine, a first-line therapy. That stopped working fairly quickly, so my healthcare team prescribed topiramate. It worked for me until recently when the flare-ups became more frequent. That meant my healthcare team needed to move me on to step 2 in my journey: Botox combined with medication.
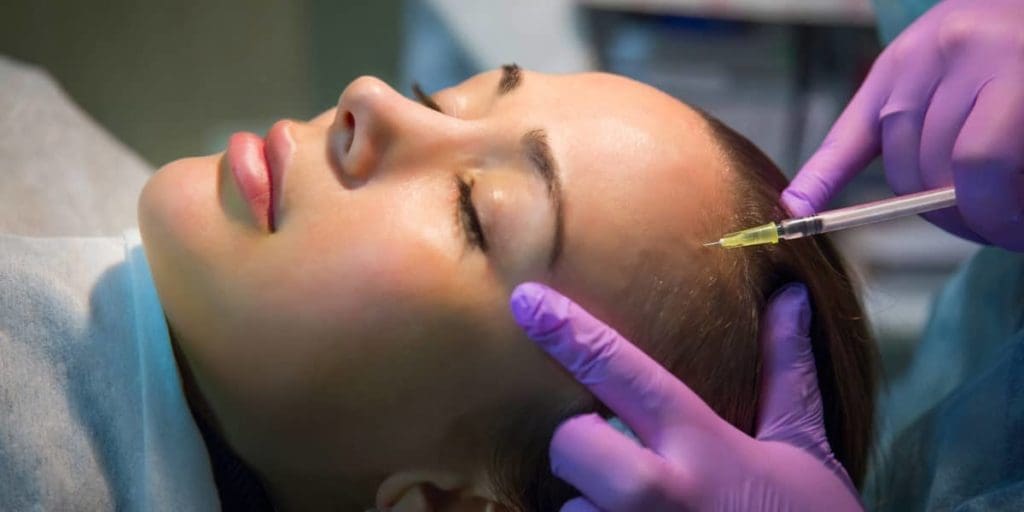
Botox aka Botulinum toxin type-A can be an effective treatment for trigeminal neuralgia. Because of my particular symptoms, my healthcare team injects Botox along my hairline on the right side near my eye. It’s never injected directly into the nerve, as there is too much potential for drooping and paralysis.
Some patients receive immediate relief; some feel relief after a month or longer. For me, it took almost 6 months before my flare-ups abated, but that relief didn’t last very long. A major – and quite unexpected – wave of pain hit me during a severe back spasm. That powerful combination landed me in the hospital. I hate going to the hospital in the first place, and this particular experience happened on a weekend motorcycle trip with my husband. Needless to say it was a disappointing end to a great trip.
When one of these flare-ups hits me, the pain begins as a mild ache just under my cheekbone. It then spreads to my eye socket, my sinus cavity and under my entire cheekbone. The ache is gentle at first, almost teasing what’s to come, and then metamorphoses into something relentless. There’s no one place to pinpoint where the pain is at that point. It’s just there, and it offers no break. It feels like tiny little hammers are striking me – not quite enough that the actual strike is painful, but that the endlessness of it is. There’s also no rhyme or reason on how long it’s going to last. Sometimes it’s 30 minutes. Sometimes it’s 12 hours.
And when it’s finally over, it feels like I’ve been punched in the cheek over and over and over, but the bruises are all on the inside. The gentlest touch on my skin is agony, yet at the same time all I want to do is press my fist into my face as hard as I can. There’s a reason it’s called the suicide disease.
I’ve reached the point where I’m considering a referral to a neurologist. There are a few procedures that can be done at that level of healthcare, with the two most popular surgeries used today being Gamma Knife radiosurgery and microvascular decompression surgery. Both are different in their approaches, but both can have excellent results. It may seem weird for those who don’t live with trigeminal neuralgia that brain surgery is a consideration for something affecting the face. But those of us who do live with it are chasing relief, and we know this level of treatment may be what ends that chase.
The fight for trigeminal neuralgia awareness


I can almost guarantee you that somebody you interacted was fighting an invisible illness be it trigeminal neuralgia, fibromyalgia, arthritis or something else. That is why I started advocating for those of us who live with invisible illnesses every day: to spread awareness about the growing number of us who are living in chronic pain, the reality of what we face every day and the importance of recognizing our struggles.
We want so badly to be seen as normal (read: healthy) that we often push ourselves far beyond our limits. You may not recognize the lengths we go to just to fit in. Or you may not see us at all, as some of us may not be healthy enough to venture out in public much anymore.
I loathe trigeminal neuralgia and all invisible illnesses that my dear friends and I live with day in and day out. I hate that we are living in pain with no end in sight. But I’m glad that more and more people are learning about us and want to know more about our illnesses and how they can help us. I’m thankful I get to play a role – however small it may be – in raising awareness about us and in fighting for more effective treatments .
To my fellow fighters: remember that there is always hope.
Would you like to share your testimony and experience about fighting chronic pain or another health condition?
Let us know by emailing us at info@painresource.com.
Are you on Facebook?
Join our online community by clicking here.






I have worked with TN patients for almost 25 years as a patient advocate and forum monitor for online peer to peer support groups. I was on the Board of the US TN Association (now re-branded as the Facial Pain Association) in the late 1990s, and contributed to increasing the visibility of TN as a disorder. I continue to support TN patients and others dealing with chronic pain. My recent published work can be found in a google search for “The Lawhern Files”. I can also be found easily on Facebook. Feel free to reach out.