Is your skin sensitive or does it hurt to touch all of a sudden? Let’s explore possible causes and treatments for sensitive skin.
Skin Sensitive To Touch Overview
Since your skin is the largest organ in your body, chronic pain in that region can become a huge nuisance. Many different conditions may contribute to sensitive skin. However, it can be hard to figure out just why your skin feels sensitive or even painful. Here’s a look at some conditions that can make your skin sensitive to touch all of a sudden, so you can find the treatment option right for you.
One Cause of Sensitive Skin Could be Shingles
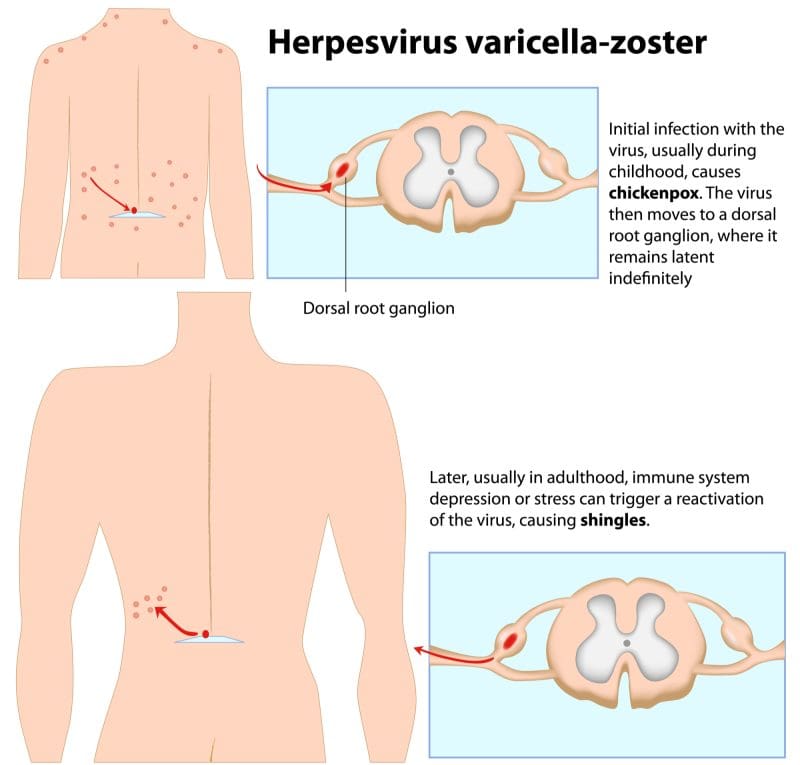
Firstly, shingles, an infection from the chickenpox virus (varicella-zoster virus), causes a very painful, blistery rash. After you’ve contracted chickenpox, the virus remains inactive in your body. Later in life, the inactive virus may reactivate, turning into shingles (herpes zoster).
If you are over 40 years of age and have been exposed to the chickenpox virus, you are at risk for developing shingles. Increased risk factors include being older than 50 years of age and having a weakened immune system.
The shingles rash may be located anywhere on your body, but most commonly wraps around your torso. In addition, symptoms normally only affect one side of your body, often in a band across your skin. In some cases, you may experience postherpetic neuralgia, one of the most common complications of shingles. This may cause burning pain in your skin long after the shingles rash has disappeared.
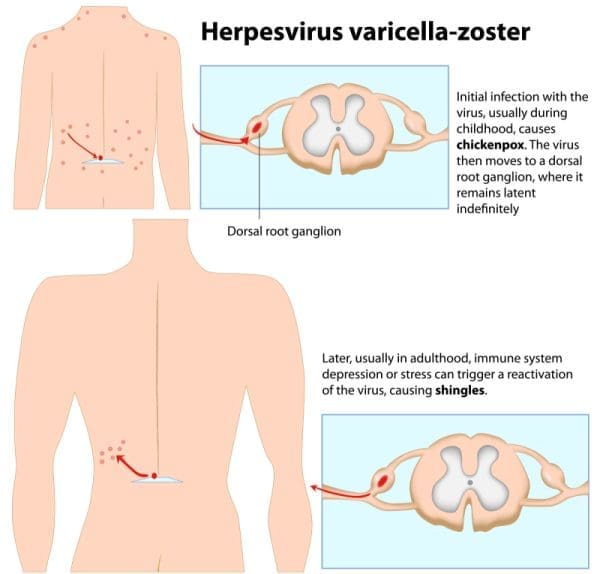
Common shingles symptoms include:
- Sensitivity to touch
- Pain, burning, numbness or tingling
- A red rash that starts a few days after the pain begins
- Itching
- Blisters that fill with fluid, open up and then crust over
Other shingles symptoms include:
- Fever
- Headache
- Light sensitivity
- Fatigue
Shingles symptoms manifest in people differently and the pain may be very intense. While a painful rash is common, some people never develop it.
If you suspect you have shingles, contact your doctor right away. It’s especially important to seek medical help if you:
- have a rash around your eye or a widespread rash
- are over 60 years old
- have a weakened immune system
Common treatments for skin pain due to shingles include:
- antiviral medications (acyclovir, valacyclovir, and famciclovir)
- pain-relieving medications ( OTC acetaminophen)
- home remedies (wet compresses, calamine lotion, and colloidal oatmeal baths)
Fibromyalgia Can Make Your Skin Sensitive to Touch
Sensitivity to touch due to tactile allodynia, thermal allodynia or mechanical allodynia is a common symptom of fibromyalgia. When you have allodynia, your body sends pain signals from non-painful stimuli. In fact, even lightly touching your skin can feel unbearably painful.
Another common symptom is a tingling sensation. That tingling feeling might be in one specific area or widespread over your body. As with any chronic health condition, certain things may trigger your fibromyalgia symptoms to worsen, causing increased skin sensitivity.


Other fibromyalgia symptoms include:
- Pain
- Numbness and tingling in hands, arms, feet, and legs
- Fatigue and problems sleeping
- Concentration and memory problems (a*k*a fibro fog)
- Body stiffness
- Headaches
- Irritable bowel syndrome
- Problems urinating
- Painful menstrual cramps
- Anxiety or depression
Typically, fibromyalgia occurs with other types of health conditions, such as migraine headaches, autoimmune diseases, chronic fatigue syndrome, and irritable bowel syndrome. Often, fibromyalgia symptoms improve once other health conditions are addressed.
Common treatments for skin pain due to fibromyalgia include:
- lidocaine and pregabalin
- NSAIDs
- electrical stimulation and hypnotherapy
Autoimmune Diseases
Autoimmune diseases occur when your immune system mistakenly attacks your body. These conditions are systemic, affecting the entire body. Often, autoimmune diseases that don’t directly affect the skin may cause skin sensitivity or redness. These autoimmune diseases include:
- Rheumatoid arthritis
- Lupus
- Thyroid diseases (Graves’ disease)
However, some types of autoimmune diseases directly affect the skin. For example, psoriasis and psoriatic arthritis are examples of autoimmune diseases that directly affect the skin. These conditions cause a build-up of skin cells that may appear scaly and red. Approximately 30% of those living with psoriasis develop psoriatic arthritis, an inflammatory form of arthritis.
Common psoriatic arthritis symptoms include:
- Fatigue
- Pain, tenderness and/or swelling in tendons
- Swollen fingers and toes
- Stiffness, pain, throbbing, swelling and tenderness in one or more joints
- Reduced range of motion
- Morning stiffness and tiredness
- Nail changes
- Redness and pain of the eye, such as conjunctivitis

See your doctor regularly and talk about your skin symptoms. Your autoimmune disease treatment plan may need to be modified if skin pain is an issue.
Common treatments for skin pain due to autoimmune diseases include:
- NSAIDs
- Disease-modifying antirheumatic drugs (DMARDs)
- Immunosuppressants
- Steroid injections
- Biologics
- Topical treatments (topical corticosteroids, vitamin D analogues, anthralin, topical retinoids, calcineurin inhibitors, salicylic acid, coal tar, moisturizers)
- Light therapy
Skin Sensitive to Touch, Dermatitis?
Dermatitis is a general term covering different types of skin inflammation. Typically, dermatitis causes an itchy rash and swollen or red skin. For instance, eczema, dandruff, and allergic reaction rashes are all forms of dermatitis.
If you come into contact with something you are allergic to, you may have an allergic reaction. Hives, a common skin condition from an allergic reaction, can cause an itchy and painful rash. Anytime you have or suspect an allergic reaction, it’s important to see your doctor or go to an urgent care clinic immediately.
Common treatments for skin pain due to dermatitis include:
- corticosteroid creams, gels or ointments
- phototherapy
- antihistamines
- topical antiseptics
Having skin sensitive to touch may be a sign of an underlying condition, such as some of the ones mentioned here. However, there are many conditions that may cause sensitive skin. It’s important to talk with your doctor about your skin sensitivities and other symptoms, so you can get on the right treatment plan.





Is there any remedies? My skin sensitivity started before COVID. It started on my right thigh and has moved up. Sometimes my face, arms, and breast. I’ve had test done and the specialist can not figure out why. He wants me to have an MRI of my back to rule that out. Anyway it’s been years and it seems there’s no end. I’ve read every post but haven’t come across a solution….there isn’t one????
Someone below named Richard mentioned calendula cream. I am wondering if you have tried infrared therapy? (It’s a painless therapy that is being studied for use in various fields of medicine.) Actually, you can buy these machines online.
I got covid last year in the summer, my main symptom was that my skin all over was so painful to the touch, I could barely put clothes on, it felt like I can had my skin ripped off of me, however when my covid went so did this symptom. However now I get it randomly but mostly when I’m feeling under the weather and it’s 10 times worse than when I had it with covid. I no longer have the sensation all over, but in random spots, for a week I’ve had the painful skin on my right arm, it feels like I have fallen and scraped my skin. Does anybody know what this could be…I am so stressed and down with it!
Hello. I am experiencing the same thing. I got Covid on Feb 18, 2023. And now on my right side of my face it is doing the same thing you are describing. I thought maybe it was shingles or bells palsy, but no. IDK what is going on.
If you received the covid vaccine(s) it(they) must be factored in as a possible cause.
The back of one hand would hurt terribly if it was lightly brushed. Boiron calendula cream has been amazingly effective for me.
How am I dealing with it….. Not very friggin well!!! It feels like I fell off a truck, got run over by several more trucks, and skidded into a gooseberry bush before being set upon by wolves. My doctor is a friggin maroon and so I had to buy Tylenol #4s on the street. I cant even work or do a git damn thing without taking one sometimes. I got home from work and had to take one and sit down and wait for it to kick in before taking off my boots and having a shower et c. Mainly in the fingers and elbows and knees and lower legs and back. The fingers are the worst. I touch the tops at all and I get shooting pain I imagine this is what it would feel like to have some cartel thug torture you by putting hot needles under your nails and into your finger joints and what not.. Anyways if you got any ideas . I never felt this before mayne Nibember thus year. I’m 35 not super good shape but not fat or unhealthy . I’m going to lose my mind this is absolute BOLLOCKS
My arms and legs are very sensitive and I cannot stand having anything against my skin. Clothing makes miserable . I can’t call it pain and I can’t call it itching. Feels like I was rubbed raw with sandpaper. No one knows what to do and I really can’t take this much longer.
That’s exactly how I feel
Diane,
I take Ibuprofen when I have a flare-up. However, my pain comes and goes and usually somewhere from the waist down (it seems to pick and choose different places). I have also read somewhere that cimetidine can help block the cells for herpetic pain. I keep a bottle of that as well to help hasten the flare-up. I have broken by tailbone a few times and no telling what else I have messed up over the years. I am also currently on Cymbalta so i feel like the flare-ups are not as often as they used to be.
This is how I felt for 5 months last year. I also described it as being rubbed with sandpaper and clothing was unbearable. It went away after the fifth month. I steal feel sensitive towards certain fabrics and wishing the last couple of weeks I’ve been feeling the sensitivity again. I have to turn my clothes inside out because of the seams.
It is apparent that this is common, reading these past posts, but I haven’t heard answers. This odd skin sensation literally makes me uncomfortable in my own skin. I can deal with it, but I worry about further development of whatever this nerve thing is. It feels awkward and unusual, but not like an actual pain. But that is what I fear, increase in intensity.
It is apparent that this is common, reading these past posts, but I haven’t heard answers. This odd skin sensation literally makes me uncomfortable in my own skin. I can deal with it, but I worry about further development of whatever this nerve thing is. It feels awkward and unusual, but not like an actual pain. But that is what I fear is an increase in intensity of pain.
Like a bad sunburn?
Like scratching a sunburn