Anti-Arthritis Plan Overview
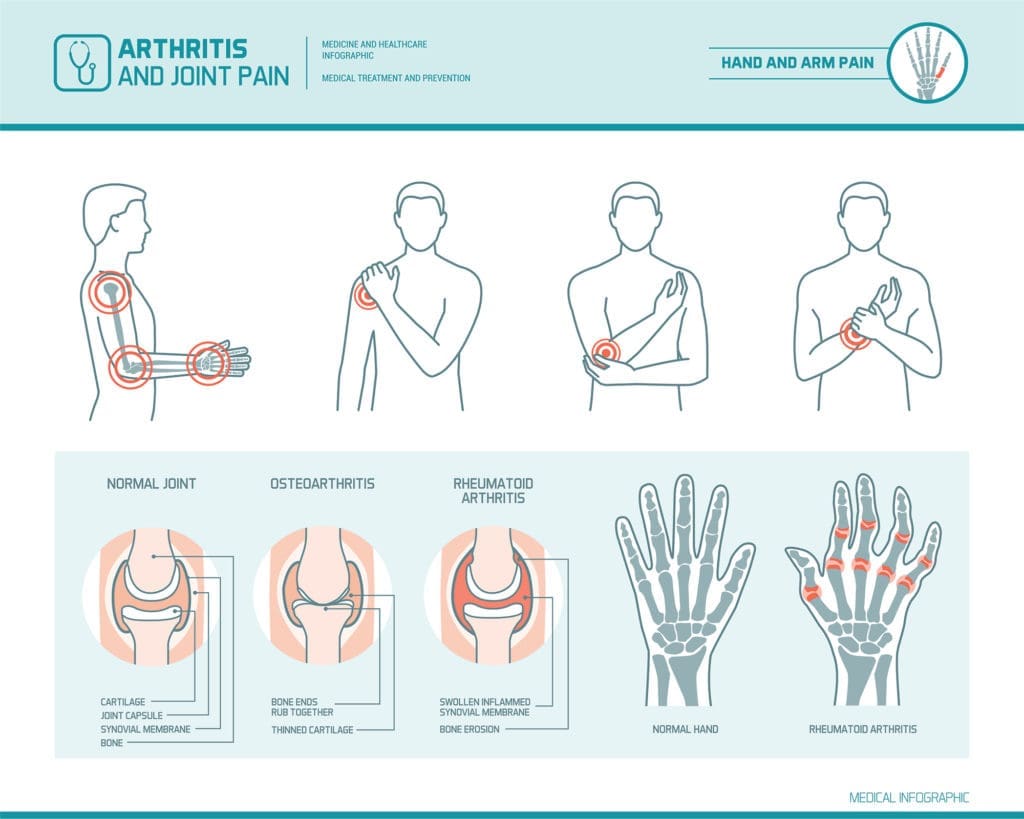 For the more than 46 million people in the United States living with arthritis, life means some amount of pain most days, and, for some, every day. With so many millions affected, it’s little surprise to hear that arthritis is the top cause of disability in the U.S.
For the more than 46 million people in the United States living with arthritis, life means some amount of pain most days, and, for some, every day. With so many millions affected, it’s little surprise to hear that arthritis is the top cause of disability in the U.S.
Even if you’re dealing with it yourself, you may not realize that joint pain is a symptom in over 100 distinct medical conditions, all of which fall under the broad umbrella of arthritis. And maybe you don’t know that that persistent ache costs us, as a country, roughly $128 billion annually in medical care and indirect costs, according to the Centers for Disease Control and Prevention (CDC).
That makes arthritis among the biggest healthcare problems in the U.S, outranked only by diabetes and heart disease. It’s not a static problem, either, says Kevin Fontaine, Ph.D., assistant professor of rheumatology in the department of medicine at Johns Hopkins University, in Baltimore. The number of people living with arthritis is growing by 750,000 people each year, and as the population gets older that number is just going to get bigger. The implications in terms of medical, economic and quality-of-life issues are enormous.
Unlike big killers such as cardiovascular disease and diabetes, though, arthritis is anything but silent. Patients describe it as sharp, stabbing, achy, intense, throbbing and notoriously hard to treat. It’s always there, says Pat Conger, 68, who has been living with osteoarthritis (OA) in her right wrist and hand for a decade. Sometimes it’s just a dull ache that feels kind of like having a cramp, and sometimes it’s so bad it feels like someone stuck a thousand pins in my hand every time I move it even a little bit.
That’s the bad news. Here’s some encouraging news: If you have arthritis you know that analgesics and NSAIDs (non-steroidal anti-inflammatory drugs) are typically a first line of defense against the hallmark symptoms of arthritis: inflammation and the dull, persistent ache of damaged joint tissue.
Fortunately, arthritis medications have gotten better over the past decade. That’s thanks largely to the debut of biologic response modifiers (often called biologics) like Humira (adalimumab) and Enbrel (etanercept), which treat different types of arthritis and work by blocking the chemicals that trigger inflammation.
Also, new surgical techniques and materials are part of physicians arsenal, like meniscus transplants used in knee arthroscopy to slow the progress of OA, and new materials such as highly cross-linked polyethylene, a long-wearing, flexible polymer used to replace damaged joints. This all makes for a much brighter picture for those hoping to ease their arthritis pain and slow the condition’s progress and damage.
Even better, there’s a lot you can do on your own to take control, says Dennis Boulware, M.D., a rheumatologist in Honolulu, and a member of the board of the American College of Rheumatologists. Patients often have more power than they think they do to change the way they feel.
Relief from arthritis shouldn’t be all about medical treatment, not by a long shot: A study published in the Journal Arthritis & Rheumatism suggests that a combination of medication and lifestyle changes could significantly reduce the annual cost of treating OA alone.
Here is an anti-arthritis plan and some proactive ways you can start easing your aches and protect yourself against more pain in the future.
Anti-Arthritis Plan – Talk about it
Even when you don’t have anything nice to say about how you’re feeling, speak up anyway. In a study, fewer than half of participants with osteoarthritis said they had talked to their rheumatologist about pain-relief options during their last visit.
Your rheumatologist won’t know your medication isn’t working or your pain regimen isn’t giving you the relief you need unless you tell him, says Carmen R. Green, M.D., a pain specialist at the University of Michigan Health System’s Center for Interventional Pain Medicine, in Ann Arbor, Michigan.
The best way to treat your arthritis symptoms isn’t written in stone; it changes over time and better relief may be as simple as switching from one analgesic to a different one, or trying a new exercise plan.
Pay attention to posture
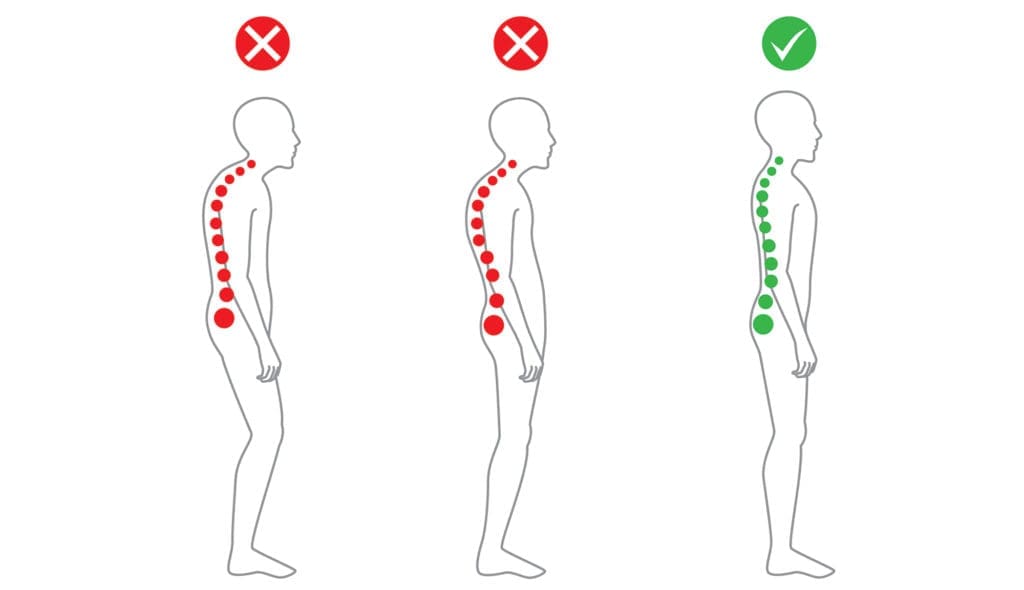

Someone with OA in their right knee, for example, may compensate by putting pressure on the joints of the left leg, which can eventually cause those joints to deteriorate.
“do something every day, even if you start with just a few minutes of an easy walk at lunchtime or a short bike ride after work”
Anti-Arthritis Plan – Move your body
Exercise is the single best thing any person with arthritis can do to relieve pain, says Leigh Callahan, Ph.D., Director of the Multidisciplinary Clinical Research Center’s Methodology Core at the Thurston Arthritis Research Center, University of North Carolina at Chapel Hill. Callahan was also the lead author on a 2009 study that found that eight weeks of exercise combining range-of-motion and flexibility moves with light resistance training improved pain, mobility and flexibility for the 347 participants with arthritis.
Even better, the relief was immediate and long-lasting; many participants in the study reported having less pain six months later. That’s just another study in a long list showing the good effects of exercise on arthritis pain, says Callahan.
Some likely benefits: Those who are at a healthy weight will see improvements in flexibility and stamina and less joint pain, fatigue and depression. And if you’re overweight, moving your body regularly obviously makes it easier to shed excess weight. Every 10 pounds you lose takes 30 to 60 pounds of pressure off the joints in your knees.
Callahan recommends range-of- motion exercises combined with yoga or tai chi, both of which mix flexibility and muscle function with low-impact exercise. Other good options to try are walking, swimming and water aerobics. The most important thing, says Callahan, is to do something every day, even if you start with just a few minutes of an easy walk at lunchtime or a short bike ride after work.
Don’t push yourself or your joints beyond your comfort level, she advises. The point is to help the pain, not to cause pain. If it hurts, stop and rest your body or do something else. Make your goal to work up to 30 minutes of exercise daily, including 10 minutes of range-of-motion moves.
What do you include in your Anti-Arthritis Plan ?
Tell us about them in the comments!
What topics related to arthritis would you like to see us explore?
Email us at info@painresource.com with your ideas.
Are you on Facebook?
Join our online community by clicking here.
Pain management starts and ends with health care awareness and dedication. Click here to read more.




