National Diabetes Month Overview
November is National Diabetes Month, a time for communities across the country to work together and raise awareness for diabetes and its impact on millions of Americans. Over 30 million adults in the United States have diabetes, and 1 in 4 don’t know. Most of us have heard of the disease and may even have some familiarity with what it is, but there are many misconceptions about the different types, causes and prevention and treatment measures. And unless we live with diabetes every day or know someone who does, we may not understand how challenging managing diabetic pain can be. Let’s explore more about this chronic disease, steps we can all take to lower our risk for type 2 and gestational diabetes and debunk common myths.
Diabetes 101
- Type 1 diabetes is an incurable autoimmune disease, but it is treatable.
- Type 2 diabetes develops when your body doesn’t use insulin well, but can often be prevented or delayed with healthy lifestyle changes.
- Gestational diabetes develops in pregnant women who have never had diabetes and usually goes away after the baby is born but increases the risk for type 2 diabetes later in life.
- Type 2 diabetes is the most common form of the disease.
- Insulin is a hormone made by the pancreas that allows your body to use sugar (glucose). That sugar comes from carbohydrates in the food you eat for energy or to store glucose for future use.
- If your body fails to make enough insulin (or fully utilize it), sugar builds up in your blood.
- Having too much sugar in your blood for long periods of time can cause serious health problems like damaging the vessels that supply blood to vital organs.
National Diabetes Month: Avoiding complications
Awareness initiatives such as National Diabetes Month are vital to public health. They emphasize the need for getting a proper diagnosis, establishing a treatment plan, considering lifestyle changes, managing diabetic pain, protecting yourself from dangerous complications commonly associated with the disease.
For example, if your body isn’t producing enough insulin and sugar remains in your blood, then it’s not being delivered to your body’s cells for energy. If you don’t have enough insulin, your body will begin using fat for energy since it doesn’t have glucose. This process releases chemicals called ketones into your blood and they can cause your blood to become acidic.
Too much acid in the blood throws off the body’s chemical balance. It’s particularly dangerous for people with diabetes. This condition is called diabetic ketoacidosis and can lead to coma or death. Luckily, it’s treatable with an insulin therapy plan, but this is why people with diabetes can’t shirk management of the disease, even when they’re on vacation or sick with the flu. It’s a life-changing diagnosis.
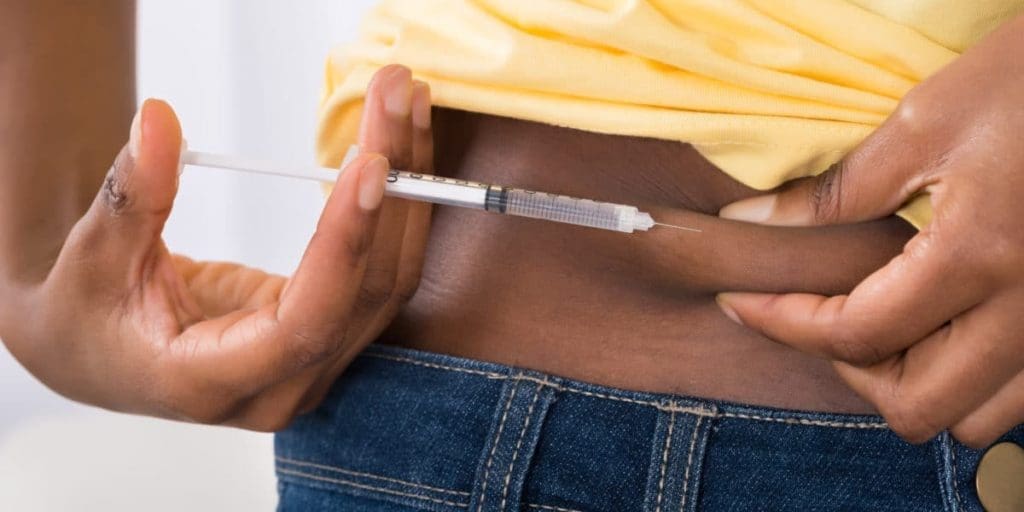
Facing diabetic nerve pain
Even if people with the disease are diligent about their insulin therapy, they still face the challenges that often come with managing diabetic pain and facing other symptoms like diabetic neuropathy that causes nerve pain all over your body. There are four types of diabetic neuropathy, but peripheral neuropathy is the most common. This is the result of nerve damage caused by high blood sugar levels and it usually affects the feet and legs.
In addition to the discomfort, nerve pain and numbness, diabetic neuropathy can lead to more serious problems like amputation, especially in older adults. One report by the American Diabetes Association shows that over 100,000 people in one year were hospitalized for diabetes-related lower-extremity amputation, a rate of 5 per 1,000 persons with diabetes.
Diabetes leads to these neuropathies due to “elevated blood glucose glycates the nerves, arteries, white blood cells and the skin, which essentially sugarcoat the structures and cause your body to stop relaying pain messages correctly.
Those who live with diabetes may also experience vascular problems. This is due to high blood glucose levels disrupting blood vessel function, and that impacts “blood flow, oxygen and nutrients going to the foot.” This means a simple cut or blister on your foot – that you can’t feel – could be left untreated and get infected. This can become serious if the infection becomes septic or tissue is severely damaged.

Living with chronic pain symptoms
Diabetic neuropathy like peripheral neuropathy can worsen slowly over time; by the time you begin to notice the pain, your nerves may have already been damaged. Living with nerve pain can make life miserable, which is even more unfair for people who are already changing their lives to manage their diabetes.
Nerve pain varies from person to person, so the best thing you can do is have an honest dialogue with your doctor to figure out a pain management or treatment plan. Diabetic nerve pain symptoms can range from numbness, tingling, burning sensation to increased sensitivity to touch and sharp pains.
Pain can be managed with strict control of your blood glucose levels, a healthy lifestyle, exercise and proper self care. There are also different types of medication and treatments that can ease the pain. The good news is nerves do have the ability to regenerate if the conditions are optimal, so relief is possible.
Debunking common diabetes myths
One of goals of National Diabetes Month is to debunk the myths, so let’s take a look at the three most popular misconceptions about diabetes:
Myth #1: I’m a healthy weight, so I can’t get diabetes.
Fact: There is a connection between your weight and type 2 diabetes, but it’s important to remember that genetics and other lifestyle factors can also play a role.
Myth #2: Diabetes is caused when people eat too much sugar.
Fact: Consuming excess calories clearly contributes to becoming overweight, a factor that is associated with type 2 diabetes. But sugar itself is not the singular cause of diabetes. Type 1 diabetes is the result of genetics and other factors. Type 2 diabetes is the result of a combination of genetics and lifestyle factors.
Myth #3: If I have diabetes, I should avoid eating carbs and sweets.
Fact: Those living with diabetes should follow the same plant-based diet recommended for the general public, including unrefined (or complex) carbs that offer nutritional density. It can include refined carbs and sweets, but in moderation and in small portions. Optimal carbohydrate counts vary by person, fitness level, etc.

Diabetes has affected lives for centuries, but there are still many unknowns about the disease. We’re still learning more every day about causes, risks and prevention tips. Recent research shows that signs of type 2 diabetes can be observed 20 years before the diagnosis and that consumption of animal products and dairy are linked to diabetes. This is vital information that can help guide lifestyle choices for the millions fighting this disease.
Understand diabetes risk factors, first steps after a diagnosis and how to protect yourself from complications with National Diabetes Month resources online.
What tips would you share with those who want to better manage their diabetic pain?
Tell us below in the comments!
What topics related to National Diabetes Month and pain caused by the disease would you like to see us research?
Email your ideas to info@painresource.com.
Are you on Facebook?
Join our online community by clicking here.





